Diabetic Eye Screening in Singapore
Diabetes is a common disease that may result in complications in the eyes. One of the most common diabetic eye diseases is diabetic retinopathy. This is because changes occur mainly in the retina, the light-sensitive layer at the back of the eye responsible for vision. When you are experiencing signs of diabetic retinopathy, it’s essential that you undergo a diabetic eye check-up. That way, the specialist in Singapore can provide you with solutions on how to manage your condition and avoid severe vision issues.
What is Diabetic Retinopathy?
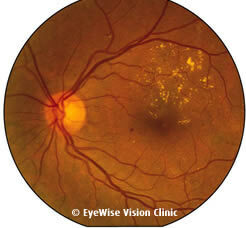
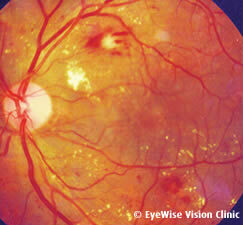
Diabetic retinopathy happens as a result of prolonged elevated sugar levels in the blood, the delicate blood vessels in the retina become fragile and start to leak fluid and proteins into the retinal tissue. This causes swelling of the retina (see Fig 1), especially in the centre area (macula) where vision is most detailed, resulting in blurred vision. Other changes in the retinal blood vessels lead to the narrowing and closure of some of the smaller blood vessels, causing insufficient blood supply and resulting in parts of the retina being starved of oxygen and nutrition. When they lack oxygen, these areas of the retina can be detected by the eye surgeon during routine eye screening tests (see Fig 2), but will not be noticed by the patient until it is too late.
This is why when you have diabetes, you must undergo regular diabetic retinal screenings in Singapore to detect earlier signs of diabetic retinopathy, even when there are no changes in vision yet. Additionally, diabetics are also more highly susceptible to cataracts and glaucoma. These can then be addressed at an earlier stage.
Types of Diabetic Retinopathy
There are two main stages of diabetic retinopathy:
Non-Proliferative Diabetic Retinopathy (NPDR): NPDR represents the initial stage of diabetic ocular disease. It occurs when small blood vessels in the retina leak, causing swelling. If this swelling affects the macula, it leads to macular oedema, a primary cause of vision loss in diabetic patients. Without treatment, as more blood vessels become blocked, the condition can progress from mild to severe.
Proliferative Diabetic Retinopathy (PDR): PDR is the more advanced and serious stage of diabetic retinopathy. It develops when damaged blood vessels close off, prompting the growth of new, fragile blood vessels in the retina. These vessels may leak into the vitreous, the clear, jellylike substance in the center of the eye. Over time, scar tissue from these new vessels can cause the retina to detach. Additionally, if the new blood vessels interfere with the normal drainage of fluid from the eye, it can increase intraocular pressure, potentially leading to glaucoma. If you experience symptoms of glaucoma, it is crucial to consult a glaucoma specialist in Singapore.
Causes and Symptoms of Diabetic Retinopathy
Diabetic retinopathy can manifest through several symptoms, including blurry or wavy vision, dark spots or strings, areas of vision loss, poor color vision, and flashes of light. These symptoms indicate that diabetes may be affecting your eyes, making it crucial to undergo regular diabetic eye screenings.
The primary cause of diabetic retinopathy is excessive sugar in the bloodstream, which can obstruct the small blood vessels that supply nutrients to the retina. In response, the eye attempts to grow new blood vessels, but these vessels are often poorly developed and prone to leaking, leading to the progression of diabetic retinopathy.
Several factors can increase the risk of developing diabetic retinopathy, including high blood pressure, high cholesterol, pregnancy, and tobacco use. Therefore, in addition to regular diabetic eye screenings and check-ups in Singapore, it is vital to maintain a healthy lifestyle to prevent the onset or progression of this condition.
Diabetic Eye Screening
The diabetic eye screening process is a non-invasive and relatively quick procedure that is essential for individuals with diabetes, particularly those who have had the condition for an extended period. The examination primarily focuses on assessing the health of the retina—the light-sensitive tissue located at the back of the eye. By closely examining the retina, the professional diabetic screener can identify any anomalies or abnormalities, such as the presence of microaneurysms, haemorrhages, or the formation of new blood vessels.
Early detection through regular diabetic eye screening tests enables healthcare providers to intervene promptly and effectively. Maintaining regular appointments for screening ensures that any changes in the eyes are identified at the earliest possible stage. That way, your eye specialist can adjust your treatment plan accordingly.
Treatment for Diabetic Retinopathy in Singapore
If your diabetic retinopathy test indicates that your disease has progressed to a later stage, then you will be given treatment, and our eye specialist will inform you. Treatment usually involves the laser and is mainly of 2 types: Central (macular) laser and Peripheral laser (what surgeons call PRP or pan-retinal photocoagulation).
Central Laser: Central laser treatment targets vessel leakage around the macula, the area responsible for detailed vision. The procedure aims to reduce fluid leakage, thereby improving retinal swelling. Multiple sessions, scheduled over separate appointments, are typically required to complete the treatment.
Peripheral Laser: Peripheral laser treatment focuses on reducing the retinal tissue that isn’t receiving sufficient oxygen. By decreasing the oxygen demand in less crucial areas of the peripheral retina, the treatment helps preserve overall vision. Like macular laser treatment, peripheral laser treatment usually requires several sessions to be fully effective.
- Pattern Scanning Laser: Our eye care clinic has access to and uses a pattern scanning laser from OptiMedica, which completes the treatment in much less time and with NO PAIN, compared to conventional Argon or standard treatment lasers. If you have been treated with a conventional laser for diabetic eye disease before, this is a completely different experience.
Diabetic Retinopathy Surgery: Preparation, Recovery & Potential Risks
Preparing for diabetic retinopathy surgery involves comprehensive eye examinations to evaluate the severity of the condition and determine the most suitable surgical approach. Patients may be required to provide a detailed medical history, undergo diagnostic tests, and adhere to specific pre-surgery guidelines. These preparations ensure that the surgery is tailored to each patient’s unique needs and health status.
Post-surgery, following the prescribed guidelines is crucial for a smooth recovery. Patients will receive instructions on medication use, eye care, and activity limitations to support the healing process. Regular follow-up appointments are essential for monitoring progress, addressing any concerns, and making adjustments to the recovery plan as needed.
As with any medical procedure, diabetic eye surgery comes with potential risks and side effects. It’s important to discuss these with your eye specialist before the surgery to understand and manage any potential complications. The medical team will take extensive measures during the procedure to minimize risks and ensure your safety.
Read More
About Dr Christopher Khng
Dr. Christopher Khng specialises in Complex Cataract and Anterior Segment Reconstruction Surgery, in particular, Iris Reconstruction and Surgery for Aniridia. His other areas of expertise include Complex Lens surgery, New Lens and Phacoemulsification technologies, Refractive surgery, Phakic IOLs (the Implantable Collamer Lens, ICL), and small-incision, topical anaesthesia phacoemulsification cataract surgery.
He completed his first two years of medical undergraduate studies at Aberdeen University, Scotland (UK). Because of cost, he completed his medical degree of MBBS at the National University of Singapore (NUS).
Dr. Khng served as Registrar, then Associate Consultant Ophthalmic Surgeon at the Singapore National Eye Centre (SNEC). Following his stint in SNEC, Dr. Khng was a Consultant at The Eye Institute, Tan Tock Seng Hospital, Singapore.
Over the years, he has worked with numerous diabetes patients during his years of practice, providing them the care they need to manage and prevent diabetic retinopathy. He has also volunteered at Community Centres to perform eye screening services, including diabetic eye screenings.

Dr Christopher Khng
MBBS, M.Med(Ophth), FRCS(Edin), AMS(Ophth 2003) Consultant Ophthalmologist
Frequently Asked Questions
It’s recommended that people with diabetes regularly see an eye doctor, so they can assess if they’re at risk of diabetic retinopathy. That way, they can take proactive measures to prevent its progression and affect their vision.
Diabetic eye screenings and general eye screenings are similar in a lot of ways, but the big difference is that diabetic eye check-ups focus more on the condition of your retina and how the blood vessels are in your eyes. Our diabetic eye screener will use fluorescein angiography to identify if you have any damaged blood cells in your eyes, as well as check your pupil dilation.
If left untreated, diabetic retinopathy can advance to more severe stages due to prolonged damage to blood vessels in the retina. Elevated blood sugar levels can cause blood vessels to leak, leading to swelling and impairing vision. As the disease progresses, abnormal blood vessel growth occurs, potentially causing retinal detachment or glaucoma. Without intervention, these complications can impact vision and even lead to blindness.
Diabetics face a higher risk of cataracts and glaucoma due to metabolic changes and prolonged exposure to high blood sugar levels. Cataracts, clouding the eye’s lens, occur earlier in diabetics. High blood sugar can lead to structural changes in the lens of the eyes over time and promote the development of cataracts. Glaucoma is characterised by optic nerve damage, which can develop due to altered blood flow and increased eye pressure from diabetic retinopathy.
Central (macular) laser treatment targets the central part of the retina (macula) to reduce swelling and leakage from abnormal blood vessels. This approach aims to preserve central vision critical for reading and recognising faces. Peripheral laser treatment, on the other hand, is focused on the outer areas of the retina to slow down the progression of abnormal vessel growth. The distinction lies in the specific areas of the retina targeted, reflecting different goals in managing diabetic retinopathy.
Individuals with diabetes should undergo diabetic eye screening tests at least once a year. However, the frequency might increase if signs of retinopathy or other eye issues are detected. Regular screenings enable early detection and intervention, significantly reducing the risk of severe vision problems. Timely adjustments to treatment plans can be made based on the progression of the disease and individual risk factors.
Lifestyle changes that can lower the risk of diabetic retinopathy include maintaining stable blood sugar levels through proper diabetes management. This involves following a balanced diet, engaging in regular physical activity, managing weight, and taking prescribed medications. Avoiding smoking and controlling blood pressure is also crucial. Consistent eye care, including regular check-ups, aids in timely detection and treatment.
While complete prevention may not be guaranteed, the risk and impact of diabetic retinopathy can be reduced through proactive measures. Optimal diabetes management is key, along with regular eye screenings and prompt treatment when necessary. Monitoring blood sugar levels, blood pressure, and cholesterol contributes to overall eye health and reduces the risk and severity of diabetic retinopathy.